Are You Overlooking Your Mid-Level Donors? Here’s How to Prioritize...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Five Crisis Communications Best Practices for Higher Education Leaders to...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
New Year, Same Annual Fund: How to Develop Fresh Messages...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Smart Year-End Giving Options to Explore with Your Donors While...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Leveraging AI for Donor Pipeline Development: Practical Strategies for Fundraising...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Build a Robust Corporate Giving Program for Impact and Sustainability...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Establishing Effective Major Gift Metrics for Your Independent School In...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The Call for Donor Engagement: Why It’s Time to Rethink...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
How to Build a Planned Giving Culture – and Why...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Keys to Developing a High-Value Fundraising Programme: Insights for Global...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Prioritize These Capabilities in Principal Gifts Fundraising For those institutions...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Three Essentials for a High-Performing Principal Gifts Team As wealthy...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Prospect Development: Rethink How You Categorize Prospects Prospect development teams...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Increasing Alumni Participation in Annual Giving is Still a Great...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Three Key Takeaways for Arts and Cultural Institutions from the...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Develop a Major Gifts Program That Attracts Ongoing Investment I...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
CRM Systems and Change Management: 3 Principles to Help Your...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Donor Qualification: How to Get the Meeting and Attract Future...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
How to Fundraise without a Fundraising Staff Attracting and retaining...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Four Essentials for Strengthening Relationships with Your Board and Volunteers...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Is it Time to Make a Change? Four Steps Every...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Strengthening Fundraising Partnerships in the C-Suite: Keys for Development Officers...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Fundraising for Social Justice: 5 Keys to Success for Museums...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Strengthen Your Campaign Planning: Leveraging Provosts as Key Advancement Partners ...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The AI Revolution and Its Implications for Advancement Teams With...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
How UK Charities Can Demonstrate ROI in Their Fundraising Programmes ...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Analytics: The Data You Need to Strengthen Your Advancement Program ...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
High-Impact Donor Stewardship: Value Your Donors and Advance Your Fundraising...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
3 Keys to Guide Your 2023 Communications Strategy It’s the...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Combat “Donor Fatigue” with These Tips to Revitalize Your Fundraising...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
How to Make Your Annual Fund Appeals More Appealing (and...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Maximize Year-End Giving in an Unpredictable Economy Regardless of how...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Our Top 5 Thought Leadership Articles of 2022 As a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Principal gifts are more than just bigger major gifts. They...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Refocus Your Independent School Advancement Team on Metrics That Matter ...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
As with many nonprofit organizations, independent schools rely on a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Gifts of appreciation for a donor or member’s generosity can...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
As women’s share of national wealth grows and their impact...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
GG+A Note: This post was originally published in May 2020...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Despite ongoing gains with improving diversity, equity, and inclusion in...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Earlier this year, I had the opportunity to speak with...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Fundraising institutions such as academic medical centers have become increasingly...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
At Grenzebach Glier and Associates, we believe that fostering an...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
How Advancement Professionals Can Leverage a Methodological Approach to Affecting...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The question of whether annual giving days have exhausted their...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
As fundraisers, we hear with some frequency from trustees and...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
We often see development office activity slow down after the...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Donors’ gifts to your organization are signs that they have...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Events have long been an important component within our fundraising...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
It’s been easy for institutions to get swept up in...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Here are three lessons we learned last month: Mentorship conversations with...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Issues matter more than ever. That’s the takeaway from a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Managing a development program is fraught with challenges. Add on...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
We’re in the midst of a moment of dramatic change...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Here are four lessons we learned last month: Our...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This Thursday will mark the conclusion of the CASE Summit...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The pandemic has had a profound impact on many people’s...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Here are four lessons we learned last month: 12% of annual...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Essentials of a Well-Planned Annual Fund: Hope Is Not a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
It's hard to overstate the importance of end-of-year giving. Nearly...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
You don’t need to be the most colorful writer to...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Here are four lessons we learned last month: Now is a critical...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Most major gifts don’t just happen. They stem from years...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Whether an institution has a reliable base of volunteers that...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The COVID-19 pandemic drove an influx of new donors to...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Washington, DC is abuzz with the Democrats’ race to pass...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Here are four lessons we learned last month: The Olympics provide a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
High employee turnover is a serious problem that has serious...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Feasibility study results are dependent on the donors who are...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The COVID-19 pandemic presented a shocking stress test to nonprofit...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
There’s a lot more to annual giving than meets the...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Volunteers want to help. They want to contribute to your...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Here are five lessons we learned last month: Overall giving...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Ensuring that donors are satisfied with their giving experience is...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The COVID-19 pandemic fundamentally altered the way that many of...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Overall giving reached $471.44 billion in 2020, setting a new...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
(Editor’s note: This article originally appeared in the Chronicle of Philanthropy)...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Do you have ambitious campaign aspirations but not much experience...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Grenzebach Glier and Associates believes that fostering a diversity of...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Here are four lessons we learned last month: Behind every...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
What inspires parents to volunteer? Keeps them engaged? Makes them...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Academic medicine and healthcare institutions have unique opportunities to leverage...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Many of us have been remotely engaging our boards for...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Here are four lessons we learned last month: It is...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Volunteers are the lifeblood of nonprofit institutions. They are often...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Note: This article originally appeared in the Spring 2021 issue...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
We’re in the midst of a significant moment for planned...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
If all goes according to plan, the United States will...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Here are four takeaways we learned last month: A good...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Campaigns are longer than ever. The median capital campaign spans...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Too often independent schools take a “tent-like” approach to major...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In a little more than a decade, GoFundMe has grown...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Whether in a campaign or not, the board of trustees...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Here are five lessons we learned last month: Comprehensive fundraising...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Over the course of 25 years in fundraising, I’ve collected...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Anyone who works in higher education knows that leadership changes...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Your board of trustees has just approved a proposed capital...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Boards can serve an extremely important role within a nonprofit...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
A number of university advancement leaders have recently asked me...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Andy Shaindlin, Vice President for Alumni Relations, recently spoke with...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In the course of a few days in March, the...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Here are four lessons we learned in January: Advancement officers...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
When most people look back on their university days, they...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Treasure Valley Family YMCA CEO David Duro was floored when...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
During my 35-plus years in development I’ve held fast to...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Let’s imagine a common scenario. Soon you’ll be sending an...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Montgomery College, a three-campus community college, in December 2019 received...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Raising money in the midst of a global pandemic and...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Only eight months into the leadership gifts phase of its...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In the webinar “Virtually Interactive Homecoming From Home” Kutztown University...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Even in normal times, institutions are likely to know far...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Along with other facets of Advancement, the pandemic has deeply...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
It’s November: time for most annual giving directors to be...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
We live in the age of personalization. Whether donors are...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
GG+A President Suzanne Hilser-Wiles recently appeared on “The Development Debrief”...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
It’s easy to count inputs. That’s why nonprofits have long...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
With the world changing at a rapid pace, there has...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
October’s outlook on fundraising has remained somewhat steady with September...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
There is growing recognition inside academia that solutions to both...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Whether you are an advocate or a skeptic of strategic...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Looking out 90 days, just eight (8%) of respondents see...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Senior Director of Annual Giving Nicole Brennan, CFRE and Program...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The global pandemic, recession, and racial reckoning have challenged nonprofits—particularly...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Nonprofit institutions have never experienced anything like the last six...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
It is difficult to escape the reality that these are...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
What would you think if I told you in December...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Alongside “COVID-19” and “pandemic," it is reasonable to assume that...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
September responses show a slight downturn in the 30, 60,...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The fall term is upon us and COVID-19 still looms....
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This is the third article in a three-part thought leadership...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Congratulations. You made it through FY20. Perhaps your school’s fundraising...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Loyola University Maryland’s Terrence Sawyer, J.D., Senior Vice President Advancement,...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In this week’s survey of fundraiser outlook, we learn that...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This fall will look dramatically different from any previous year....
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Jim McKey, GG+A Senior Vice President, and University of Dayton’s...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This is the second article in a three-part thought leadership...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
An email from your CRM vendor states that it suffered...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This is the first article in a three-part thought leadership...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Kate Azizi, Vice President for Institutional Advancement at the Medical...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In the webinar, "Fundraising campaigns in the time of COVID-19,"...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In August, more advancement offices have reopened for in-person work...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The COVID-19 pandemic has left the fundraising world reeling. As...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
At roughly the same time that the pandemic forced much...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Engaging our constituents has always been at the heart of...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
John Glier, GG+A CEO, and Mark Luellen, Vice President for...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In week 17 of the SurveyLab tracking of fundraiser outlook,...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
COVID-19 and its economic aftermath have caused a brute reckoning,...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In this webinar, GG+A’s Dan Lowman and Adrian Salmon walk...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In this week’s SurveyLab tracking of fundraiser outlook, participants demonstrated...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Carnegie Mellon’s take on Giving Tuesday, #givingCMUday, has been an...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The COVID-19 pandemic forced advancement teams to pivot abruptly to...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Mexico’s largest private, nonprofit university system, which encompasses 25 campuses...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Prior to the COVID-19 pandemic, most higher education institutions recognized...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
You did the impossible. Overnight, you pivoted from donor events,...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In normal times, fundraising follows a consistent path. While the...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Like many universities, Rice University has focused on its commitment...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This post was updated on Aug. 17. In this webinar,...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The 30-day high impact to fundraising jumped this week to...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
When you look in the mirror in the morning, do...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Early this spring, seemingly overnight, the time-tested habits of Advancement...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Fundraising outlook overall continues to improve, while crowdsourcing and giving...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
When a recent mini campaign planning study at Harvard T.H....
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The internet’s ability to maintain connections has been crucial to...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Negative fundraising outlooks for the next 30, 60 and 90...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
New Zealand is ahead of the pandemic curve compared to...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
GG+A's Independent Schools practice recently hosted a webinar highlighting how...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Fundraiser outlook over the next three months is holding steady,...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Editor's note: This statement was issued on behalf of GG+A...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Earlier this week, GG+A’s leadership put out a statement addressing...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The 30-, 60-, and 90-day fundraising outlooks have found a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In the webinar, "Stewardship During the COVID-19 Pandemic and Beyond,”...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The fundraising outlook for the next 30, 60, and 90...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In November 2011, I was finishing my 15th year as...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
I’ll start by saying: look, I get it. We’ve all...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In the webinar, "Redefining How We Engage with the University’s...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In this webinar, GG+A Vice Presidents Adrian Salmon and Jason Shough...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
For the first time since tracking began, fundraising outlooks for...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In this webinar, Jeff Nearhoof, GG+A Senior Vice President, talks...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
GG+A's latest webinar features GG+A Senior Vice Presidents Melinda Church...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Editor's note: This article was updated on July 7 There’s...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Most nonprofit organizations know the benefits of performing a wealth...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Fundraising offices continue to be increasingly positive in their outlook...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
How are nonprofits—from local arts organizations to major research universities—staying...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Last month, GG+A hosted the webinar, “How Arts and Cultural...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Throughout the current crisis, GG+A's team has been responding to...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In college, I was fortunate enough to spend a semester...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The social and economic issues brought on by the pandemic...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
While your zoo, aquarium, museum or cultural institution may be...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Fundraisers were slightly more optimistic this week than last, according...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Editor's note: This article was updated on May 29 We’ve...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In this webinar, GG+A CEO John Glier talks to Anthony...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
On April 17, GG+A hosted a webinar with guest Marc...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In this webinar, GG+A CEO John Glier talks to Cindy...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Most organizations think of data governance as just another thing...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Robert J. Spiller, Assistant Secretary for Advancement for the Smithsonian...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In this webinar, "Impact of COVID-19 on Higher Education: Immediate...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The outlook for fundraising is turning more negative after four...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This unprecedented health and economic crisis that we are all...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Editor's note: This post was updated on June 11, 2020....
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In this webinar, Marc Weinstein, Vice-Principal of University Advancement at...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Sentiment for the next 30 and 60 days out continues...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
It’s challenging to navigate the philanthropic landscape amid a global...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Editor's note: This is Part II of a two-part response...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Editor's note: This is Part I of a two-part response...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Crises strike every organization. Data systems are breached. Research protocols...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In late February, the NorthShore University HealthSystem Foundation team was...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Fundraiser sentiment has been steadily improving since the beginning of...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Since my last blog post, my GG+A colleagues and I...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
As our academic medical centers, health care systems, and community...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Independent schools face unique challenges, and this remains true during...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
GG+A Vice President Adrian Salmon recently conducted a webinar on...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Nonprofit organizations are becoming increasingly comfortable with remote activity and...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
GG+A’s latest webinar, “Fundraising for the Nation’s Museums: Planning and...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
One of the more recent casualties of COVID-19 in the...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Most of us have seen the recent reminders on social...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Small development shops know how important and transformational planned gifts...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Most nonprofit organizations have moved to a fully remote development...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
GG+A's latest webinar, “Making Relationships Matter: UCLA Advancement Program’s Response...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In the wake of the COVID-19 crisis, the team at...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Unsurprisingly, there are high levels of concern and uncertainty across...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
I’ve spent the past week reaching out to my annual...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
As nonprofits scramble to navigate the current crisis, the team...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
COVID-19-related news is producing tremendous uncertainty. There’s so much information...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
(Editor's note: This article originally appeared in the Chronicle of...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Five principles to guide advancement professionals as you reach out...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
One day. 4,995 donors. $1,164,487 raised to fund programs, teams,...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
University of Pennsylvania Law School will lead students and alumni...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Employees who have no chance to utilize newfound knowledge forget...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
GG+A has partnered with institutions around the globe helping them...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Grenzebach, Glier and Associates CEO John Glier joins a distinguished...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
On June 9, 2019, hundreds of thousands of Hong Kong...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The American Association of Art Museum Curators recently released their...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Nonprofit Research Collaborative has released their Winter 2019 survey report. ...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The new Schwartz Reisman Innovation Centre will turbocharge the next...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This article is the seventh and final installment in a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In addition to the many valuable new features in DonorScape...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This article is the sixth installment in a series. Read...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This article is the fifth installment in a series. Read...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This article is the fourth in a series. Read more...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Mary K. Carrasco, Assistant Head of School for Advancement at...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
DonorScape quickly identifies top donor prospects for efficient fundraising, but...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This article is the third installment in a series. The...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This article is the second installment in a series on...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
What organizations help you connect with fellow fundraising professionals in...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This is the time of year when many people think...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Donors overwhelmingly report that they are not seeing the impact...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
“Hong Kong overtook New York to become the world’s largest...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Hi, my name is Casey. I’m the new business development...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In 2016, President Tim Sands of Virginia Tech set a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The University of Calgary (UCalgary) launched Energize: The Campaign for...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
GG+A’s Survey Lab has developed a Donor Experience Scorecard that...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The future is female, or at least the future of...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Nancy Gillece leads Hood College’s Office of Institutional Advancement, which...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
It is no secret that social media is becoming an...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The Segerstrom Center for the Arts “believes in the power...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Women’s boards represent a unique fundraising institution with a long,...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Giving USA noted that in 2017, corporate giving grew at...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Nestled in the Blue Ridge Mountains of northwestern North Carolina,...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
For a long time, the word “alumni” referred only to...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
A new survey of 231 college administrators conducted by the...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
If you had a chance to tune into GG+A’s recent...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Donor segmentation is not a new concept for most nonprofit...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The Giving Institute and Giving USA Foundation recently brought together...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Connecting to the ever-growing millennial donor population has been a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In 2005, Thomas L. Friedman told us "The World is...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
As I watched a recent CBS 60 Minutes segment, I...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
By Rachel Schwimmer In a time of unpredictable government economic...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The rally cry for data was loud and clear at...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
By Rachel Schwimmer - A recent GG+A Survey Lab study...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Respondents are very philanthropic and plan to be so in...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
At some point in our careers, it is inevitable that...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
By Rachel Schwimmer According to a new study by GG+A...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
By Rachel Schwimmer A new GG+A Survey Lab study finds...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
By Felipe Hernandez A new GG+A Survey Lab study finds...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
A new study by the GG+A Survey Lab finds that...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Strong, effective stewardship programs are a core element of fundraising...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
If you work with prospects in their late 60s or...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
It was the memo heard around the world. In December...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Most fundraisers and their managers very appropriately have their eye...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Earlier this year, the Council to the Aid of Education...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
A few months ago, an independent school client asked us...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Purdue University: A case study in sustaining fundraising success through...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Imagine that you’re a development director and manager for a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
A client recently wanted to produce a data visualization that...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
“You know I love the school, but I just can’t...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The number of financially independent, separately incorporated alumni associations has...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
“Does it sing and dance?” With a piercing glance, my...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
This article is based on a presentation developed for Building...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
International fundraising can complement an organization’s traditional efforts and greatly...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
“It is a far, far better thing that I do,...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In December 2016, the Information Commissioner (UK) fined the RSPCA...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
I am privileged to work with a diverse array of...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Animals can’t raise money to help protect their habitats, improve...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Predictive analytics streamlines and complements prospect research. Yet it can...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In decades of working with premier fundraising organisations worldwide and...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Thank you to all who could join GG+A last night...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In the first two blog posts of GG+A’s Ross-CASE Survey...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In our previous Ross-CASE blog, my colleague Adrian Salmon...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Recently my GG+A colleagues and I presented our analysis of...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Supplemental data is available for just about anything you might...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Some years ago when I was an experienced gift officer...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
With enormous time commitments, a wide variety of duties, and...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
I once had a conversation with a prospective donor who...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
After three years of anticipation, the San Francisco Museum of...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The list of skills gift officers must possess is a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
A few days ago, Shakespeare fans around the world united...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
GG+A Vice President Adrian Salmon will present a day-long workshop...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The independent school sector has a multitude of opportunities to...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
CASE social media leaders and practitioners who gather this week...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Prospect Wealth Ratings can be tremendously valuable in setting the...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
According to a 2015 study by the National Endowment for...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
My GG+A colleagues in the US have been taken aback...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Andrew Gossen, Senior Director for Social Media Strategy, Alumni...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
By Ken Ashworth, Former Senior Vice President, Training and...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Last week I attended the CASE-NAIS annual conference in New...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
By Suzanne Hilser-Wiles Planning for the CASE NAIS conference this...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Is it possible to prove the value of alumni relations?...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Regular giving is now most definitely multi-channel. The mean number...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Defining alumni relations can help us articulate our purpose--and help...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
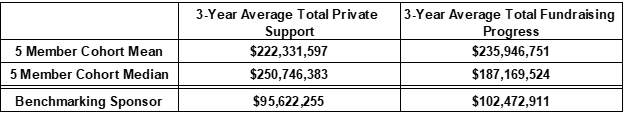
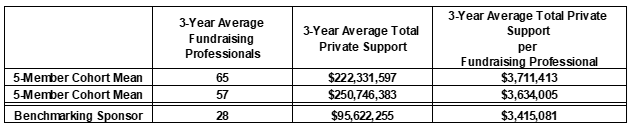
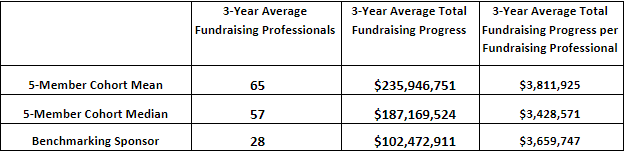
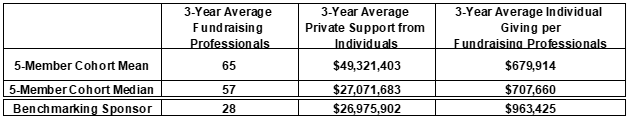
One of the most common reasons our clients ask for benchmarking...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
In partnering with their development colleagues in fundraising initiatives involving...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Recently, the notion of international markets as a growth opportunity has taken hold...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
"The new regulations have been tightened as a result of...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
“Our challenge is to build a prospect pool that is...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
You're the type who never gives up. But sometimes, letting...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Studies show that people around the world are naturally inclined...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
A data collection technique that forces respondents to choose a...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The Giving USA 2015 Report on Philanthropic Giving, the annual report on...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The Giving USA 2015 Report on Philanthropic Giving, the annual report on...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The Giving USA 2015 Report on Philanthropic Giving, the annual report on...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The Giving USA 2015 Report on Philanthropic Giving, the annual report on...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The more I peruse the literature on women’s philanthropy, the more...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
First you gotta crawl, then walk… and then you can...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
How can a small development team with a big fundraising...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
As news is created and distributed at a previously unimaginable...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
So many museums suffer what some might consider a “happy...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
The term “big data” may be the buzz word of...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
Effective case statements consist of compelling prose that, while appealing...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png
I am a sports fan (or fanatic, some might say);...
Grenzebach Glier & Associates Inc
http://gga.ugmade.co/wp-content/themes/gga/assets/img/grenzebach-glier-and-associates-print-only.png